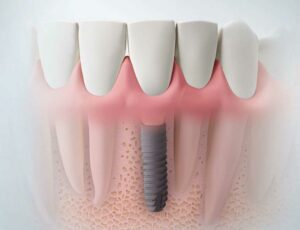
After your surgery for a new dental implant, you may experience bleeding or a blood clot, which are normal. However, if you have dental implant bleeding years later, it can be a sign of infection or other kinds of damage. This issue needs to be taken care of immediately.
Causes of Bleeding Around Implants
There are two causes of dental implant bleeding — mucositis and peri-implantitis. Mucositis is a reversible condition that affects the soft tissue around the implant. It is caused by:
- Bacteria.
- Excess cement from the crown placement.
- Poor oral hygiene.
Unchecked mucositis can cause peri-implantitis, which is more severe and destructive. This form of gum disease affects both the soft tissue and bone around the implant. Peri-implantitis can be caused by:
- Genetics.
- History of periodontitis.
- Ill-fitting restorations.
- Inadequate oral hygiene.
- Poorly managed diabetes.
- Smoking.
- Strong force when biting.
- Extra cement below the gum line on a cement-retained restoration.
Patients with peri-implantitis usually have an infection as well.
Symptoms of Mucositis and Peri-Implantitis
The symptoms of the conditions that can cause a bleeding implant are often recognizable. However, some patients with these conditions do not experience any pain and may not know they have mucositis or peri-implantitis.
The symptoms of mucositis are inflamed, bleeding and red soft tissue around the implant. The symptoms of peri-implantitis include the same as mucositis in addition to:
- Bone loss of 2 to 3 millimeters around the implant.
- Probing depth greater than 5 to 6 millimeters.
- Bleeding after probing.
Mucositis is not an infection, but peri-implantitis is. The signs of an infected dental implant include:
- Swollen, red gums.
- Bleeding or pus around the implant.
- Bad breath.
- Pain when chewing.
- Loose implant.
How to Treat an Infection Around a Dental Implant
Dental implant bleeding must be diagnosed and treated right away. Addressing the problem early will prevent the implant from further deteriorating. When left untreated, peri-implantitis can cause implant failure.
The first step is to schedule a dentist appointment. Your dentist will examine your mouth, take x-rays and ask about other symptoms to determine the bleeding’s cause. Dentists diagnose mucositis by checking for retained cement. If excess cement caused mucositis, your dentist can remove it. Otherwise, mucositis is easily treatable with an effective oral hygiene plan that includes brushing, flossing and water flossing. Caring for your mouth will thoroughly clean the implant’s surface and prevent bacteria from getting into the gum around the implant.
Your dentist can determine if you have peri-implantitis by checking your pocket depths. Severe cases of peri-implantitis are treated with surgery to stop the disease, grow more bone mass and save the implant. If this does not work, your dentist will remove the implant, then rebuild the lost soft tissue and bone. If possible, the dental implant can get put in later.
Learn More About Hiossen® Implant Today
Hiossen Implant has a unique and reliable dental implant design. For more information, fill out our contact form today.